Stereo Investigator Helps Uncover Autonomic Diabetic Neuropathy Link
Stomach pain, heartburn, and head rushes are frequent complaints of patients suffering from long-term diabetes. Doctors usually blame these symptoms on autonomic neuropathy, a dysfunction of the nerves that regulate blood pressure, heart rate, and digestion. But there’s really not all that much evidence out there to prove this diagnosis. Researchers at the University of Minnesota and Wake Forest University set out to discover the relationship between autonomic neuropathy and diabetes by studying mucosal nerves in the stomach.
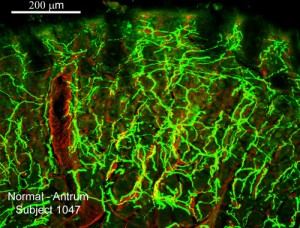
Mucosa tissue biopsies were obtained from 15 healthy control subjects and 13 subjects with type 1 diabetes, according to the paper published last month in Neurology “Gastric mucosal nerve density – A biomarker for diabetic autonomic neuropathy?” All diabetic subjects had secondary complications, which included gastroparesis. The scientists used Stereo Investigator to conduct design-based stereology to quantify the mucosal nerves in the stomachs of each subject.
“This task proved challenging, as the mucosa is heavily innervated with a network of nerve fibers, and individual axons are difficult to isolate,” said lead author Dr. Mona Selim. “By using stereology and Stereo Investigator we were able to overcome this problem and get an estimate for nerve fiber length and volume density.”
Compared to the biopsies of the control subjects, which displayed healthy results, the diabetic subjects all showed abnormal mucosal nerve fibers, including discontinuous or disorganized networks, swollen nerves, and nerve loss. Also, after overnight fasting, the stomachs of nearly all the diabetic subjects contained residual food.
Read the free abstract, or download the full paper at neurology.org
M.M. Selim, MD, G. Wendelschafer-Crabb, MS, J.B. Redmon, MD, A. Khoruts, MD, J.S. Hodges, PhD, K. Koch, MD, D. Walk, MD and W.R. Kennedy, MD, “Gastric mucosal nerve density – A biomarker for diabetic autonomic neuropathy?” (Neurology 2010;75:973-981)